Social determinants adolescent health is a concept that fundamentally challenges the idea that staying healthy is purely a matter of personal willpower. Research suggests that the environments surrounding young people — from their families and friendships to their schools, neighborhoods, and national policies — shape their physical and mental wellbeing in profound ways. A landmark study, “Adolescence and the Social Determinants of Health,” confirms that adolescent health outcomes are deeply tied to the social structures young people live within.
You might assume that health is mainly about eating well or exercising regularly — and those things certainly matter. But studies indicate that factors like access to education, income inequality, neighborhood safety, and even a country’s overall wealth can be just as decisive in determining whether a young person thrives or struggles. This article unpacks the key social forces identified in that research, explains why each one matters, and shows what we can all do — as individuals, families, and communities — to give adolescents a healthier future.
Once again, personality researcher and author of Villain Encyclopedia, Tokiwa (@etokiwa999), will provide the explanation.
※We have developed the HEXACO-JP Personality Assessment! It has more scientific basis than MBTI. Tap below for details.

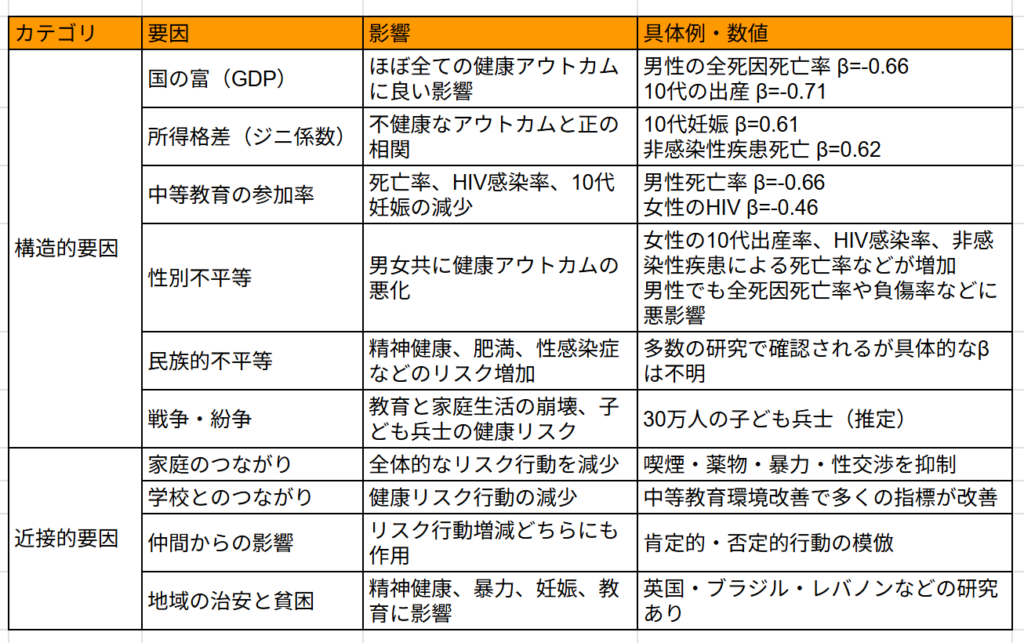
※ Summary of key concepts in this article. “Outcomes” refers to measurable health indicators that result from social, environmental, or policy conditions.
※ Specific outcomes examined in the research include mortality rates, teen pregnancy rates, HIV infection rates, non-communicable disease mortality, rates of violence and injury, and tobacco and substance use.
目次
- 1 How Family and School Relationships Shape Adolescent Wellbeing
- 2 Neighborhood, Economics, and Youth Health Inequality
- 3 National Systems and Global Forces as Social Determinants of Adolescent Health
- 4 What Individuals, Families, and Communities Can Do
- 5 Frequently Asked Questions
- 5.1 What are the social determinants of adolescent health?
- 5.2 How does family influence teen health outcomes?
- 5.3 Does income inequality directly affect teen health?
- 5.4 How do peer effects on adolescent wellbeing actually work?
- 5.5 Why is education considered an adolescent health factor?
- 5.6 Does gender inequality affect adolescent boys as well as girls?
- 5.7 What can an individual teenager do when their social environment is difficult?
- 6 Summary: Adolescent Health Is a Shared Responsibility
How Family and School Relationships Shape Adolescent Wellbeing
The Protective Power of Strong Family Connections
A warm, stable relationship with parents or caregivers is one of the single most important protective factors for adolescent health. When young people feel genuinely connected to their families, they tend to engage in fewer risky behaviors — including tobacco use, alcohol consumption, early sexual activity, and involvement in violence. The mechanism is fairly straightforward: a household that feels safe and communicative gives adolescents an emotional anchor that helps them navigate the pressures of teenage life.
Research suggests that it is not just the presence of parents that matters, but the quality of the interaction. Families where adults actively listen, set gentle but consistent boundaries, and maintain predictable daily routines tend to raise adolescents with stronger mental health and lower rates of substance misuse. Conversely, when families are under severe financial stress or parental mental health is compromised, those pressures can spill over onto teenagers, increasing emotional instability and vulnerability to risky choices.
Practical family habits that research associates with better adolescent outcomes include:
- Daily conversation: Even brief, low-pressure check-ins help teens feel seen and valued, reducing the likelihood of them seeking validation through risky peer behavior.
- Shared routines: Consistent meal times, bedtimes, and family activities create a sense of structure that supports emotional regulation.
- Gentle monitoring: Parents who are aware of their child’s activities — without being controlling — tend to see better health outcomes in their teenagers.
It is equally important to acknowledge that individual families cannot do this alone. Social support systems — affordable housing, parental leave policies, and accessible mental health services — make it easier for families to provide the stable environment adolescents need. The family home is the foundation of adolescent health, but that foundation needs community and policy support to stay strong.
Why the School Environment Is a Critical Social Determinant of Adolescent Health
Because adolescents spend a significant portion of their waking hours at school, the quality and safety of that environment has a direct impact on both mental and physical health. Schools where students feel respected, where bullying is actively addressed, and where teachers are approachable tend to produce adolescents with lower rates of substance use, violence, and psychological distress. In contrast, schools that feel unsafe or hostile can become sources of chronic stress — a well-documented driver of long-term health problems.
Studies indicate that the relationship between a student and their teacher is particularly meaningful. Adolescents who feel that at least one adult at school genuinely cares about them are more likely to attend regularly, engage academically, and avoid high-risk behaviors. This “trusted adult” effect is a surprisingly powerful buffer against the kinds of social pressures that teenagers routinely face.
The key environmental characteristics of health-promoting schools include:
- Physical safety: Buildings and classrooms that are clean, well-maintained, and free from violence set the baseline for learning and wellbeing.
- Supportive teacher relationships: Warm, consistent adult mentorship inside school is associated with reduced risk behavior outside of it.
- Anti-bullying culture: Schools that actively monitor and address peer aggression show measurably better mental health outcomes among students.
- Accessible counseling: The presence of a trusted counselor or support professional gives students a confidential outlet for stress and crisis.
Parent-school collaboration also appears to amplify these effects. When caregivers maintain an active, positive relationship with their child’s school community, students tend to feel more secure and engaged. A school that functions as a genuine community — not just an academic institution — acts as a powerful social determinant of adolescent health in its own right.
Peer Effects on Adolescent Wellbeing: The Double-Edged Influence of Friends
Adolescence is a developmental stage when peer relationships carry extraordinary weight — and the direction that influence takes can either protect or undermine a young person’s health. Research consistently shows that peer effects on adolescent wellbeing are among the strongest predictors of whether a teenager engages in risk behaviors. Friends who model positive behaviors — academic effort, physical activity, goal-setting — tend to encourage those same behaviors in one another. The reverse is equally true.
Three specific psychological mechanisms help explain why peers hold so much sway during adolescence:
- Social modeling: Teens are highly attuned to what their peers are doing, and they naturally tend to mirror those behaviors — whether healthy or harmful.
- Conformity pressure: The desire to belong and be accepted is especially intense in adolescence, making it harder to resist group norms even when those norms involve risk.
- Situational drift: Young people in group settings are more susceptible to “going along with the moment,” particularly in unstructured or unsupervised environments.
This does not mean adolescents are passive victims of their social circles. Research suggests that developing strong self-awareness and communication skills helps teens navigate peer pressure more effectively. Adults — parents, teachers, and mentors — can also play a role by expressing genuine, non-judgmental interest in a teenager’s friendships and helping them recognize both the positive and potentially risky influences in their social world. Choosing and maintaining supportive peer relationships is one of the most actionable steps an adolescent can take to protect their own health.
Neighborhood, Economics, and Youth Health Inequality
How Neighborhood Safety and Community Cohesion Affect Teen Health
The physical and social qualities of the neighborhood an adolescent grows up in are a significant — and often underestimated — determinant of their health. A community with high crime rates, few public spaces, and limited social cohesion can restrict the opportunities available to young people in ways that directly harm their wellbeing. When teens feel unsafe in their immediate environment, they spend less time outdoors, engage in less physical activity, and experience higher levels of chronic stress — all of which have measurable health consequences.
Conversely, neighborhoods with strong social capital — that is, communities where residents know and trust one another — tend to produce better adolescent health outcomes. The presence of reliable adult figures outside the family provides additional layers of support and accountability that help keep young people on track.
Characteristics of neighborhoods that tend to support adolescent health include:
- Accessible public spaces: Parks, libraries, sports facilities, and community centers give adolescents safe places to spend time and develop social skills.
- Intergenerational interaction: Events and programs that bring adults and young people together build trust and reduce social isolation.
- Community watchfulness: Neighborhoods where residents look out for one another — and for local youth — create informal safety nets that formal institutions cannot fully replicate.
Research also suggests that strong community support reinforces the positive effects of family and school environments. When all 3 layers — home, school, and community — are functioning well together, the cumulative benefit to adolescent health is substantially greater than any single factor alone. The neighborhood surrounding a young person is not just a backdrop to their life; it is an active force shaping who they become.
Socioeconomic Status and Youth Health: How Family Income Shapes Daily Life
Socioeconomic status and youth health are deeply intertwined — not just because wealthier families can afford better food or healthcare, but because financial stress ripples through the entire family system in ways that directly affect adolescents. When parents are working multiple jobs to make ends meet, the time and emotional energy available for warm, attentive parenting tends to diminish. This reduction in connection and supervision, rather than material deprivation alone, is a key pathway through which poverty harms teenage health.
Studies indicate that adolescents from lower-income households are more likely to engage in behaviors such as tobacco use, alcohol consumption, and irregular sleep patterns — behaviors often linked to stress management and reduced parental oversight rather than deliberate choice. The long-term consequences can be severe, affecting educational attainment, future earning potential, and health well into adulthood.
The specific channels through which low family income tends to affect adolescent health include:
- Nutritional quality: Healthy, varied diets are more expensive and time-consuming to prepare, making them less accessible to families under financial pressure.
- Extracurricular exclusion: Sports, arts, tutoring, and other enrichment activities — which build social skills and self-esteem — are often beyond reach for lower-income families.
- Emotional instability: Financial anxiety is contagious within households; teens absorb and internalize parental stress, which can manifest as anxiety, depression, or acting-out behavior.
Persistent poverty can also narrow a teenager’s vision of their own future, reducing the sense of purpose and hope that researchers identify as protective factors for health. Addressing family income inequality is therefore not only an economic issue — it is a foundational adolescent health issue.
National Systems and Global Forces as Social Determinants of Adolescent Health
How a Country’s Wealth and Income Inequality Determine Teen Health Outcomes
Zooming out from the individual and community level, the research makes clear that national-level economic conditions are among the most powerful social determinants adolescent health researchers have identified. Countries with higher national income tend to have more robust healthcare systems, greater access to secondary education, and more comprehensive social safety nets — all of which translate directly into better adolescent health metrics. Studies have found a strong association between national wealth (measured by GDP per capita) and lower adolescent mortality rates, particularly among young males.
However, national wealth alone does not tell the whole story. The distribution of that wealth — measured by indicators like the Gini coefficient — appears to matter just as much, if not more. Research suggests that countries with high income inequality tend to show elevated rates of teen pregnancy, higher rates of violence-related injury, and worse mental health outcomes among young people, even when the country is relatively affluent overall.
The specific advantages that wealthier, more equal societies tend to provide for adolescents include:
- Universal healthcare access: Young people can seek preventive and curative care without financial barriers.
- Higher school enrollment rates: Public investment in education keeps more adolescents in school and out of high-risk environments.
- Broader social support infrastructure: Mental health services, youth programs, and community organizations fill gaps that families alone cannot cover.
Importantly, societies with similar wealth levels can still show significant differences in youth health inequality, depending on cultural norms, political priorities, and the specific policies in place. This suggests that deliberate investment in adolescent-focused systems matters — not just passive economic growth. Reducing income inequality and directing national resources toward young people is one of the highest-return investments a society can make in its own future.
Education Access as a Lever for Adolescent Health
Access to quality education — particularly secondary education — is one of the most consistently documented adolescent health factors across all regions of the world. The research is clear: adolescents who remain in school are substantially less likely to die, contract infectious diseases like HIV, experience early pregnancy, or suffer serious injuries than their out-of-school peers. Education does not just transmit knowledge; it creates structure, instills a sense of future possibility, and places young people in environments with supportive adults and positive peer norms.
The protective effects of education on adolescent health appear to operate through several distinct pathways:
- Health literacy: Educated adolescents tend to have better knowledge of how to protect themselves from disease, unintended pregnancy, and dangerous situations.
- Delayed risk exposure: School attendance keeps young people in structured, supervised settings during hours when unsupervised teens are most likely to engage in risk behavior.
- Future orientation: Research suggests that adolescents who see a meaningful future ahead of them — with academic or career aspirations — are significantly more likely to make health-protective choices today.
Secondary school enrollment (roughly equivalent to middle and high school) appears to be a particularly important threshold. Keeping adolescents engaged through these years, and addressing the financial, social, and logistical barriers that cause dropout, is one of the most effective strategies available to governments and communities trying to improve adolescent health at scale. Investing in education is, quite literally, investing in the long-term health of the next generation.
Gender Inequality and Its Ripple Effects on Teen Health
Societies where women and girls face systematic disadvantage in education, employment, and social status tend to show worse adolescent health outcomes — not only for young women, but for young men as well. When girls are denied educational opportunities or pressured into early marriage and childbearing, the resulting health consequences are severe: elevated maternal mortality, higher rates of obstetric complications, and long-term physical and psychological harm. But the research goes further, indicating that gender inequality creates systemic instability that harms entire communities.
In societies with entrenched gender inequality, young men also tend to experience elevated rates of violence, unemployment, and substance use. This may reflect rigid cultural norms around masculinity that leave young men without constructive outlets or emotional support systems. The data suggests that gender inequality is not a “women’s issue” — it is a public health issue with consequences across the entire adolescent population.
Countries and communities with high gender inequality tend to see the following patterns in adolescent health:
- Higher female mortality and morbidity: Young women face greater health risks when social structures limit their autonomy and access to care.
- Elevated male violence and instability: Rigid gender norms often channel male adolescent stress into aggression, with significant public health consequences.
- Destabilized family systems: When either parent is denied opportunity or dignity, the entire household — and its children — suffers the downstream effects.
Promoting gender equity in education, employment, and civic life is therefore both a social justice goal and a concrete adolescent health strategy. When young women can safely study, work, and participate in society, the health outcomes of all adolescents in that community tend to improve.
The Devastating Impact of Armed Conflict on Young People’s Health
For adolescents growing up in regions affected by war, armed conflict, or civil unrest, the social determinants of health are overwhelmed in the most extreme possible way. Conflict disrupts every protective layer simultaneously: families are separated, schools are closed or destroyed, communities collapse, and economic systems fail. The physical dangers are immediate — injury, disease, and death — but the psychological wounds can persist for decades, affecting an entire generation’s capacity for trust, stability, and healthy relationships.
Research indicates that approximately 300,000 children worldwide are estimated to have been involved as child soldiers in various conflicts — a figure that illustrates the scale of developmental harm inflicted by organized violence on the young. Even adolescents who are not directly combatants experience profound health consequences from living in conflict zones, including disrupted schooling, food insecurity, sexual violence, and chronic trauma responses.
The specific ways in which armed conflict undermines adolescent health include:
- Educational disruption: Schools close, teachers flee, and the continuity of learning that protects adolescent health is shattered.
- Family separation and displacement: Loss of parental presence removes the primary protective relationship in a young person’s life.
- Forced participation in violence: Whether as soldiers, laborers, or victims, adolescents in conflict zones face exposures that cause lasting physical and psychological harm.
Recovery from conflict requires sustained, long-term investment in rebuilding all of the social structures that protect adolescent health — schools, families, communities, and institutions. Peace is not merely the absence of war; for young people, it is the precondition for health itself.
What Individuals, Families, and Communities Can Do
Understanding the social determinants of adolescent health is only valuable if it leads to action. Here are evidence-informed steps that different groups can take, along with the reasoning behind each recommendation:
For Adolescents Themselves
- Invest in your friendships deliberately. Research consistently shows that peer groups are one of the strongest influences on adolescent health behavior. Seeking out friends who support your goals and values — and gently distancing yourself from persistently negative influences — is one of the most effective health strategies available to a teenager. It works because the social modeling effect operates in both directions.
- Stay engaged with school. Even on difficult days, maintaining school attendance preserves access to supportive adults, structured time, and a sense of future possibility — all of which are documented protective factors. If school feels unsafe or overwhelming, reaching out to a counselor or trusted teacher is a concrete first step.
- Communicate openly at home. Talking with parents or caregivers — even briefly, even imperfectly — strengthens the family connection that research identifies as a primary buffer against risk behavior. You don’t need perfect conversations, just regular ones.
For Parents and Caregivers
- Prioritize connection over correction. Studies indicate that parental warmth and genuine interest in a teenager’s life are more protective than strict rules alone. The goal is to be someone your adolescent wants to talk to, not just someone they have to report to.
- Be aware of financial stress signals. Economic pressure affects the whole household. Recognizing when stress is limiting your availability and seeking support — from community resources, employee assistance programs, or social services — benefits your teenager directly.
- Stay involved with school. Even small gestures of engagement — attending school events, maintaining contact with teachers — signal to your teenager that their education matters and create accountability structures that support healthy behavior.
For Communities and Policymakers
- Invest in public spaces for youth. Parks, libraries, community centers, and organized youth programs are not luxuries — they are infrastructure for adolescent health. Communities that provide them tend to see measurably better outcomes.
- Address income inequality proactively. Policies that reduce the gap between the wealthiest and least wealthy members of society — through progressive taxation, social transfers, living wage legislation, and universal healthcare — have a demonstrated impact on youth health inequality.
- Champion gender equity in education and employment. Removing barriers that prevent girls and women from full participation in society benefits the health of all adolescents, not just young women.
Frequently Asked Questions
Social determinants of adolescent health are the environmental, social, and economic conditions that shape whether young people stay healthy. These include family relationships, school quality, peer influences, neighborhood safety, family income, national wealth and inequality, access to education, gender equity, and the presence or absence of armed conflict. Research suggests that these factors often have a greater combined influence on adolescent health outcomes than individual behaviors like diet or exercise alone.
How does family influence teen health outcomes?
Family influence on teen health operates primarily through the quality of the parent-child relationship. Adolescents who feel warmly connected to their parents or caregivers tend to engage in fewer risky behaviors — including substance use, early sexual activity, and violence involvement. Daily conversation, shared routines, and gentle but consistent parental monitoring are among the specific practices most strongly associated with positive adolescent health outcomes, according to research in this field.
Does income inequality directly affect teen health?
Yes — research indicates that income inequality is a significant driver of youth health inequality, even within wealthy countries. Societies with large gaps between rich and poor tend to show higher rates of teen pregnancy, greater youth violence, and worse mental health outcomes among adolescents. This appears to occur because inequality erodes social trust, reduces access to quality education and healthcare for lower-income families, and concentrates chronic stress among the most economically vulnerable households.
How do peer effects on adolescent wellbeing actually work?
Peer effects on adolescent wellbeing tend to operate through 3 main mechanisms: social modeling (teens naturally imitate what they see their friends doing), conformity pressure (the desire to belong makes it harder to resist group norms), and situational drift (going along with a group in the moment, especially in unstructured environments). These effects can be positive or negative depending on the peer group. Research suggests that adolescents surrounded by health-oriented friends are more likely to adopt similar behaviors themselves.
Why is education considered an adolescent health factor?
Education is considered one of the most important adolescent health factors because it simultaneously delivers health knowledge, provides structured and supervised time, connects young people with supportive adults, and builds a sense of future possibility — all of which are documented protective factors. Studies indicate that adolescents who complete secondary education have substantially lower rates of mortality, HIV infection, unintended pregnancy, and serious injury compared to those who drop out.
Does gender inequality affect adolescent boys as well as girls?
Research suggests that gender inequality harms adolescent health across the entire population, not only young women. In societies with high gender inequality, young men tend to experience elevated rates of violence, unemployment, and substance use — outcomes linked to rigid masculine norms that leave little room for help-seeking or emotional expression. This means that promoting gender equity is not just a concern for girls’ welfare; it is a broader adolescent public health strategy with benefits for young people of all genders.
Even within challenging social environments, research suggests that several individual-level actions can make a meaningful difference. Maintaining at least 1 strong, supportive relationship — with a parent, teacher, coach, or mentor — provides a crucial anchor. Staying engaged with school, even imperfectly, preserves access to protective structures. Seeking out positive peer connections and being deliberate about the social situations you participate in also reduces exposure to risk. While structural change is ultimately necessary, these personal strategies have real, documented protective value.
The evidence is both sobering and empowering: the social determinants adolescent health researchers have identified — family bonds, school quality, peer relationships, neighborhood conditions, economic equity, educational access, gender equality, and peace — are not fixed features of the world. They are conditions that families, communities, and governments shape through their choices and priorities every day. No single teenager can control all of these forces, but every adult, institution, and policy decision tilts the balance toward health or away from it.
Understanding this interconnected picture is the first step toward changing it. Whether you are a young person thinking about your own social world, a parent reflecting on what kind of home environment you are creating, or a community member considering where to direct your energy and advocacy — the science gives you a clear map. Adolescent health is not a private matter. It is a collective achievement, built layer by layer from the inside out: from the family dinner table to national policy. If this article has helped you see those layers more clearly, the next step is to ask yourself: which layer can I strengthen today?
